HRV vs Resting Heart Rate: What Each Metric Tells You, and Why You Need Both
Quick answer
Heart rate variability (HRV) and resting heart rate (RHR) are related, but they are not interchangeable. Resting heart rate tells you how fast your heart is beating at rest, while HRV tells you how much the time between beats varies from one beat to the next. In practice, RHR is an idle-speed metric and HRV is a flexibility metric. Because they reflect different parts of cardiovascular and autonomic function, they can move together or diverge, and that divergence is often the most informative signal of all. 1, 2, 3, 4, 5
What resting heart rate measures
Resting heart rate is the baseline pace your heart settles into under resting conditions. Physiologically, it reflects sinus node automaticity, plus the balance of sympathetic and parasympathetic input acting on that pacemaker system. In plain English, it is how fast the engine idles when demand is low. 3, 6, 7
Classic work by Maciel and later mechanistic work by D’Souza showed that training-related bradycardia can persist even after autonomic blockade, pointing to intrinsic sinus node remodeling, including HCN4 channel changes, as part of the story. That is one reason RHR and HRV should not be treated like copies of the same metric. 3, 6
A lower resting heart rate is often favorable in trained people, but lower is not automatically better in every context. In athletes, sinus bradycardia is often benign. In non-athletes with symptoms or medication effects, the same number can mean something very different. Elevated RHR is associated with higher long-term mortality risk, but those are cohort-level associations, not one-number verdicts. 8, 9, 10, 11
What HRV measures
Heart rate variability is not about how fast the heart beats. It is about how much beat-to-beat timing changes around the average rate. Those tiny changes reflect how flexibly the cardiovascular system is being modulated, especially by vagal input. 1, 2, 12
Two people can share the same resting heart rate and have very different HRV profiles. One may have highly adaptable beat-to-beat control, the other may have a flatter, less resilient pattern. That is why a wearable dashboard that shows only heart rate misses part of the picture. 12, 5
HRV works best when captured under consistent conditions, especially overnight, and compared against your own baseline over time. If you want the action side of that discussion, read how to improve HRV. 13, 14, 15, 16
The two-gauge cockpit, the core thesis
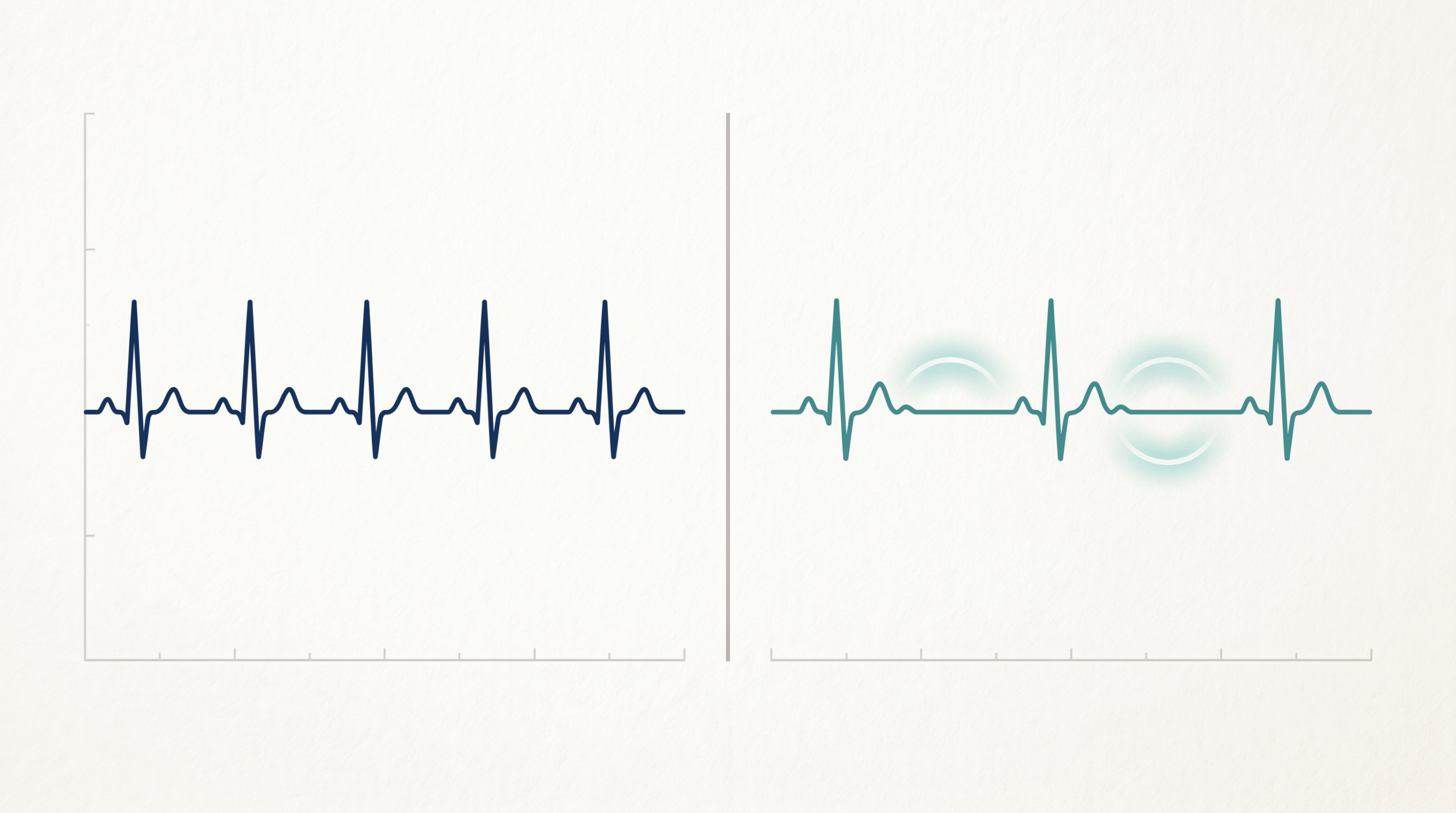
The best way to think about HRV and resting heart rate is as a two-gauge cockpit. One gauge shows idle speed, your resting heart rate. The other shows responsiveness, your HRV. You would not fly using only one dial, because one number cannot tell you both how hard the system is working and how flexibly it is being controlled. 6, 7, 4, 5
RHR can change through intrinsic sinus node adaptation, medication effects, fitness changes, and autonomic tone. HRV is more tightly tied to beat-to-beat modulation, especially vagal influence. The two gauges are connected, but not redundant. One can look stable while the other changes first. 12, 3, 6, 7
That is why dual-metric tracking can be directionally more informative than treating either signal as a standalone health score, though this additive value is mechanistically and observationally supported rather than proven by hard-outcome randomized trials in general wearable users. Emerging wearable and cohort evidence suggests that HRV and RHR together can reveal physiologic changes that one metric alone would blur. 17, 4, 5, 18
When HRV and RHR diverge
Divergence is where this topic gets useful. Many people assume lower RHR should always mean higher HRV, or that a normal RHR should cancel out a low HRV warning. Real physiology does not work that cleanly. HRV and RHR can diverge because they respond through partly different mechanisms and on different timelines. 7, 19, 4
The clearest example is beta-blocker therapy. In one longitudinal heart failure study, atenolol lowered heart rate while HRV markers such as SDNN improved over time. In a separate propranolol study in hyperthyroid patients, the same intervention reduced heart rate while increasing SDNN, RMSSD, and high-frequency HRV. Same person, same period, opposite movement. A lower RHR does not mean HRV must rise for the same reason, and an improving HRV does not mean heart rate must stay unchanged. 20, 21
You see the same principle in training and recovery. Heart rate can drop early with conditioning, while HRV may improve more gradually. During overreaching or illness, the pattern often reverses: RHR drifts up while HRV falls. In athlete-monitoring and wearable literature, that concordant worsening pattern is one of the most practical signals of incomplete recovery. It is useful because the two metrics are agreeing, but for different mechanistic reasons. 7, 22, 23, 24
Healthy physiology can also produce divergence. In pregnancy tracking with a WHOOP wearable, resting heart rate climbed while HRV declined across gestation, then recovered postpartum on different schedules. 17
If your HRV is low but your resting heart rate is still normal, the variability signal may have changed before the level signal did. If your RHR is low but your HRV is also low, context matters even more. In athletes that could reflect accumulated load or poor sleep. In non-athletes, it could reflect medication effects, intrinsic bradycardia, or measurement artifact. 10, 11, 20, 25
What the combination tells you
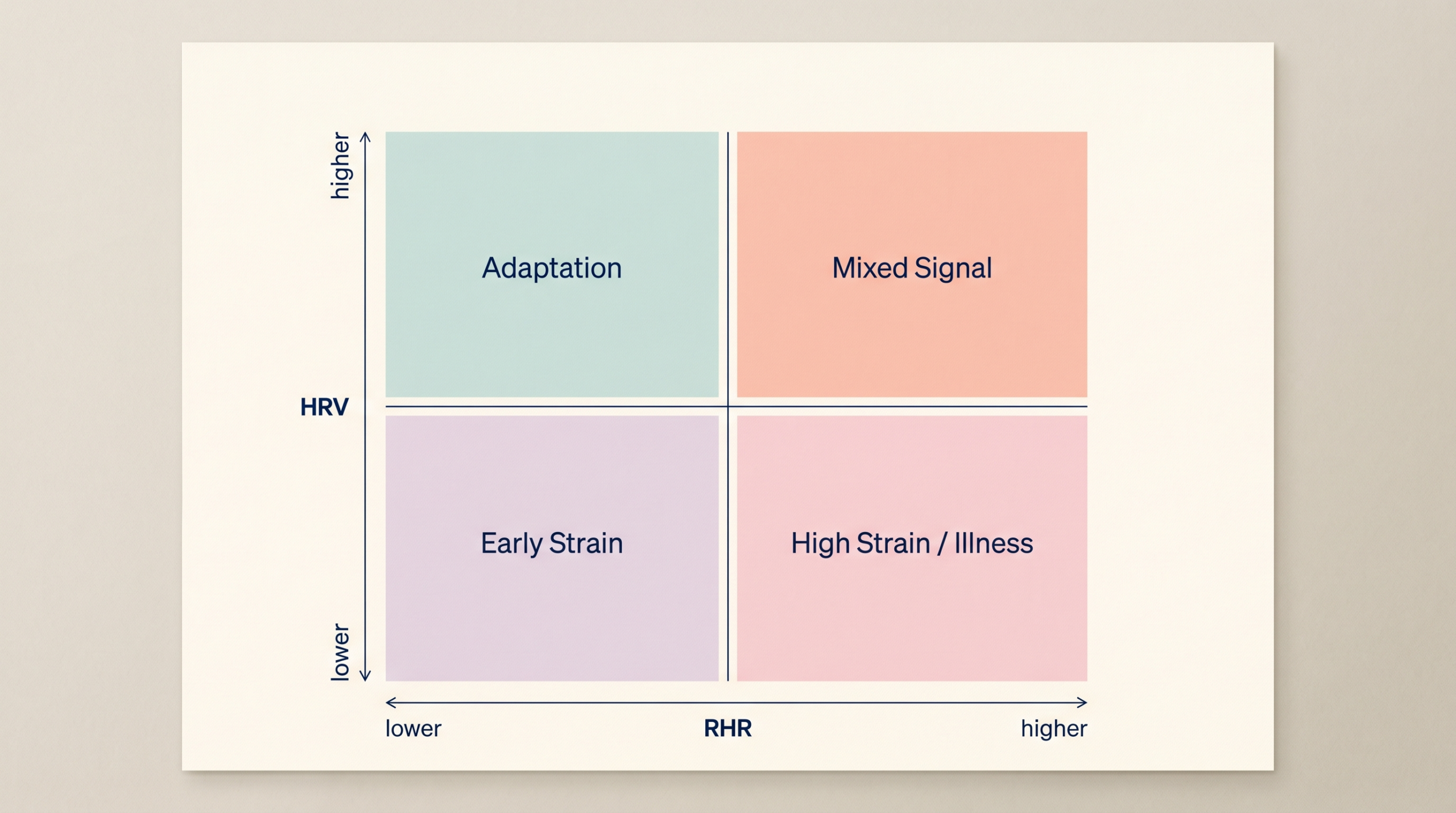
Using HRV and RHR together is less about creating a magical composite score and more about reading pattern combinations well. Concordant patterns are usually the easiest to interpret. Discordant patterns are often the most interesting. 4, 5, 18
| Pattern | Likely interpretation | Why it matters |
|---|---|---|
| HRV down, RHR up | Common strain pattern, often seen with illness, poor recovery, alcohol, or acute stress | Both gauges worsening at once increases confidence that baseline physiology is under load 22, 4 |
| HRV up, RHR down | Often seen with positive adaptation, improved recovery, or training response | Signals may be moving in a favorable direction together, though not always at the same speed 7, 26 |
| HRV down, RHR stable | Early strain, poor sleep, high load, or a change that HR has not reflected yet | Variability can move before level metrics do 13, 22, 5 |
| HRV stable or up, RHR down sharply after medication | Medication or intrinsic rate effects rather than pure fitness adaptation | The beta-blocker case is the cleanest example 20, 21 |
| HRV up, RHR still high | Partial recovery, deconditioning improving unevenly, or a high personal RHR setpoint | Better than using one metric alone, but still needs trend context 27, 28, 18 |
The value of dual tracking is that concordance and discordance help you avoid false certainty. A stable RHR does not rule out strain. A low RHR does not guarantee resilience. A high HRV does not erase symptoms or medication context. 8, 10, 20, 5
The evidence for combined interpretation is real, grounded in observational wearable work and mechanistic studies, but additive predictive value for hard clinical outcomes has not been established in randomized trials. Use these patterns as directional signals, not clinical determinations. 4, 5, 18
How to measure both accurately
Measurement quality decides whether these metrics are useful or misleading. For resting heart rate, nocturnal minimum heart rate is generally more informative than a random daytime pulse check. In the Copenhagen City Heart Study substudy, Holter-derived minimum nocturnal RHR outperformed casual ECG-based resting heart rate for predicting cardiovascular outcomes. The basic lesson is simple: stable resting conditions beat opportunistic spot checks. 29
For HRV, the most practical consumer target is nocturnal RMSSD or another overnight time-domain measure collected under low-motion conditions. Ultra-short HRV can still carry value, but wearable HRV is strongest when measured repeatedly at rest or during sleep. 13, 14, 15, 16
| Method | Best use | Strengths | Limits |
|---|---|---|---|
| ECG, multi-minute or clinical protocol | Reference measurement for HRV and rhythm assessment | Highest signal fidelity, strongest rhythm context | Less convenient for continuous everyday monitoring 13 |
| Wearable overnight PPG | Trend tracking for nightly RHR and HRV | Strong accuracy at rest, high convenience, best fit for longitudinal baselines 30, 15, 16 | Accuracy drops during movement, device methods vary 31 |
| Daytime spot-check wearable reading | Quick directional check only | Convenient | More vulnerable to motion, posture, stress, and timing noise 31 |
Wrist- and ring-based photoplethysmography (PPG) can be less accurate in people with darker skin tones, because melanin can attenuate the optical signal. Systematic review data show this affects heart rate accuracy across devices, and the same issue can affect HRV derived from PPG signals as well. Consumer wearables are most trustworthy for within-person trends under controlled conditions, not as universal substitutes for ECG. 25, 31
What “normal” looks like
There is no single normal HRV or resting heart rate value that applies to everyone. Age, sex, fitness level, medication use, sport type, and baseline physiology all shift the range. HRV norms decline with age, and differences by sex narrow later in life. In the MESA reference data and Singapore normative data, both the central values and the lower-tail cutoffs change meaningfully across groups. 32, 33
Resting heart rate is similarly contextual. Clinical normal is often given as 60 to 100 beats per minute, but that is a broad clinical reference interval, not an optimized health range. Population studies show higher RHR tracks with higher long-term mortality risk, yet very low RHR can be entirely benign in endurance athletes and potentially concerning in non-athletes depending on symptoms and history. Normal and optimal are not synonyms. 8, 9, 10, 11
A genetics sidebar helps explain why comparison across people is tricky. Twin and GWAS work show that resting heart rate has a heritable component, but most of its variance is still environmental and behavioral. Genetically elevated RHR appears to have a causal link with dilated cardiomyopathy risk, while HRV’s story is more dependent on measurement context and lived physiology than on a single inherited setpoint. That is another reason personal baseline beats social comparison. 27, 28
If you are looking for a benchmark, ask whether your own values are stable, drifting, or changing after a clear trigger such as training, sleep loss, alcohol, illness, or medication adjustment. That is usually more informative than asking whether your number is better than someone else’s. See also HRV chart by age and good resting heart rate. 32, 33
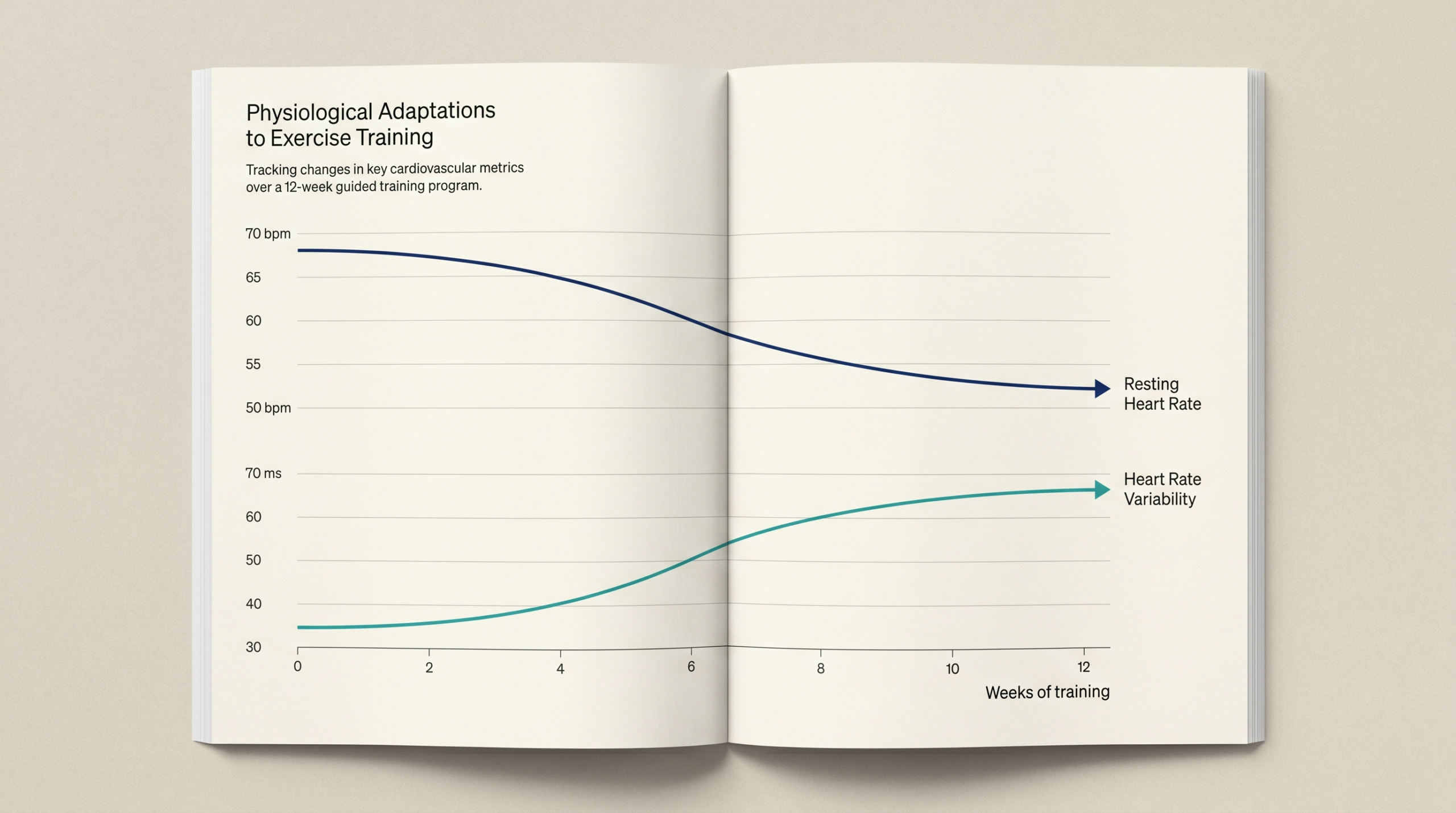
How to improve both
The levers that improve HRV and resting heart rate overlap, but the timelines do not always match. Better sleep, aerobic fitness, sensible training progression, lower alcohol intake, stress reduction, and adequate recovery can all move both metrics in a favorable direction. Exercise meta-analyses show meaningful gains in HRV, while training studies show resting heart rate often falls as conditioning improves. 7, 26, 34, 35
If your goal is practical improvement, track both metrics against sleep, stress, alcohol, and training load rather than forcing one metric to behave on command. Start with how to improve HRV and, where relevant, remote therapeutic monitoring. 23, 24, 19
Clinical caveats and disclaimer
HRV and resting heart rate are useful physiological signals, but they are not diagnostic tests on their own. A low HRV or unusual resting heart rate does not automatically mean disease, and a low resting heart rate is not always a sign of health without context such as fitness level, medication use, symptoms, and medical history. Wearable readings can also vary by device, measurement method, movement, and skin-tone-related PPG accuracy. If you have symptoms, cardiovascular concerns, or questions about how medications affect your readings, interpretation should happen with a qualified clinician.
These metrics are best used to add context, not replace clinical judgment. Elevated RHR and reduced HRV are both associated with higher long-term risk in cohort studies, and their combination can be directionally informative in conditions like autonomic neuropathy, heart failure, or recovery monitoring. But none of that means a wearable can diagnose disease or predict an individual cardiac event. 8, 9, 36, 13, 37, 18
Numbers are signals, not conclusions. 17, 20, 21, 25
FAQ
What is the relationship between resting heart rate and HRV?
Resting heart rate and HRV are linked because both reflect cardiovascular regulation, but they describe different dimensions of it. Resting heart rate is how fast the heart beats at rest. HRV is how much the timing between beats varies. They often move in opposite directions over time, but not always, because RHR is a level signal and HRV is a modulation signal. That is why using both together is usually more informative than treating one as a substitute for the other. 12, 3, 4, 5
Is HRV better than resting heart rate for measuring recovery?
HRV is often more sensitive to acute recovery disruptions, especially when measured overnight and compared against a personal baseline. But that does not make RHR obsolete. Resting heart rate can add useful confirmation, especially when it rises alongside a falling HRV. The best practical answer is that HRV is often earlier, while RHR is often simpler. Together they give a clearer picture than either metric alone, even though hard-outcome superiority of combined monitoring is still emerging rather than definitively proven. 29, 13, 22, 4, 18
Does a low resting heart rate mean high HRV?
No. A low resting heart rate does not automatically mean high HRV. Endurance training can lower RHR, but medications such as beta-blockers can also lower it, and intrinsic sinus node remodeling can lower it without producing the same change in HRV. A person can have a low RHR with only modest HRV, or a normal RHR with excellent HRV. Context, trend, and measurement quality matter more than assuming one number guarantees the other. 6, 20, 21
What does it mean if my HRV is low but my resting heart rate is normal?
That pattern often means the variability signal changed before the heart-rate level signal did. Common explanations include poor sleep, accumulated training load, alcohol, stress, or the early phase of illness or recovery disruption. It does not automatically mean disease. It means the two-gauge cockpit is giving you an asymmetric reading, and the right next step is to look at trend, symptoms, and recent exposures instead of overreacting to a single day. 22, 4, 23, 24
Which wearables measure both HRV and resting heart rate?
Several consumer wearables report both HRV and resting heart rate, including ring- and watch-based devices that use PPG during sleep or rest. The more important question is how they measure them. Overnight time-domain HRV, especially RMSSD, tends to be more reliable than daytime spot checks, and both HR and HRV accuracy degrade with motion. PPG-based optical sensors can also show reduced accuracy on darker skin tones and during motion, per recent systematic reviews 25. If you are comparing devices, prioritize measurement method, sleep capture quality, and trend consistency over dashboard polish. See wearables that measure HRV and resting heart rate. 31, 30, 15, 16
How do stress and alcohol affect HRV vs resting heart rate differently?
Stress and alcohol often reduce HRV faster and more noticeably than they change resting heart rate, especially in overnight wearable data. That is one reason HRV is often considered the more sensitive acute signal. Resting heart rate may still rise, but usually as a blunter level change. When both occur together, confidence in the interpretation goes up. When only HRV moves, that often means the system is under strain before heart rate has shifted enough to be obvious. 13, 22, 4
What is a good HRV for my age?
A good HRV for your age depends on how it was measured, how long the recording was, and which reference population you are comparing yourself to. Population norms clearly decline with age, and sex differences narrow later in life. That means a value that is ordinary at age 65 may be unusually low at age 25. The safest interpretation is to compare yourself to validated age-aware reference data and, even more importantly, to your own stable baseline over time. 32, 33
Can you have good HRV with a high resting heart rate?
Yes. A person can have relatively strong HRV for their context and still have a higher resting heart rate because the two metrics are not the same thing. Genetics, deconditioning, medications, stress physiology, and individual baseline differences can all keep RHR higher while HRV remains decent. That said, persistently elevated RHR still deserves attention because population studies link it with higher long-term risk. The right interpretation is not to pick a winner, but to understand what each metric is contributing. 8, 27, 28, 5
References
- Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Heart rate variability: standards of measurement, physiological interpretation and clinical use. Circulation. 1996;93(5):1043-1065.
- Ernst G. Hidden Signals: The History and Methods of Heart Rate Variability. Frontiers in Public Health. 2017;5:265. doi:10.3389/fpubh.2017.00265
- Maciel BC, Gallo Junior L, Marin Neto JA, et al. Parasympathetic contribution to bradycardia induced by endurance training in man. Cardiovascular Research. 1985;19(10):642-648. doi:10.1093/cvr/19.10.642
- Rowan SP, Lilly CL, Claydon EA, et al. Monitoring one heart to help two: heart rate variability and resting heart rate using wearable technology in active women across the perinatal period. BMC Pregnancy and Childbirth. 2022;22(1):887. doi:10.1186/s12884-022-05183-z
- Routledge HC, Chowdhary S, Townend JN. Heart rate variability: a therapeutic target? Journal of Clinical Pharmacy and Therapeutics. 2002;27(2):85-92. doi:10.1046/j.1365-2710.2002.00404.x
- D’Souza A, Bucchi A, Johnsen AB, et al. Exercise. training reduces resting heart rate via downregulation of the funny channel HCN4. Nature Communications. 2014;5, 3775. doi:10.1038/ncomms4775
- Yamamoto K, Miyachi M, Saitoh T, et al. Effects of endurance training on resting and post-exercise cardiac autonomic control. Medicine and Science in Sports and Exercise. 2001;33(9):1496-1502. doi:10.1097/00005768-200109000-00012
- Zhang D, Shen X, Qi X Resting. heart rate and all-cause and cardiovascular mortality in the general population: a meta-analysis. CMAJ. 2016;188(3), E53-E63. doi:10.1503/cmaj.150535
- Aune D, Sen A, o’Hartaigh B, et al. Resting. heart rate and the risk of cardiovascular disease. 2017;total cancer, and all-cause mortality: a systematic review and dose-response meta-analysis of prospective studies. Nutrition, Metabolism and Cardiovascular Diseases, 27(6), 504-517. doi:10.1016/j.numecd.2017.04.004
- Climstein M, Ranchordas MK, Huynh B, et al. Electrocardiographic. Assessment of National-Level Triathletes: Sinus Bradycardia and Other Electrocardiographic Abnormalities. Sports (Basel). 2025;13(1), 17. doi:10.3390/sports13010017
- Azevedo LF, Perlingeiro PS, Hachul DT, et al. Sport. modality affects bradycardia level and its mechanisms of control in professional athletes. International Journal of Sports Medicine. 2014;35(10), 814-820. doi:10.1055/s-0033-1364026
- Routledge HC, Chowdhary S, Townend JN Heart. rate variability: a therapeutic target? Journal of Clinical Pharmacy and Therapeutics. 2002;27(2), 85-92. doi:10.1046/j.1365-2710.2002.00404.x
- Orini M, van Duijvenboden S, Young WJ, et al. Long-term. association of ultra-short heart rate variability with cardiovascular events. Scientific Reports. 2023;13(1), 18966. doi:10.1038/s41598-023-45988-2
- Orini M, van Duijvenboden S, Young WJ, et al. Long-term association of ultra-short heart rate variability with cardiovascular events. Scientific Reports. 2023;13(1):18966. doi:10.1038/s41598-023-45988-2
- Cao R et al Accuracy. Assessment of Oura Ring Nocturnal Heart Rate and Heart Rate Variability in Comparison With Electrocardiography in Time and Frequency Domains: Comprehensive Analysis. Journal of Medical Internet Research. 2022;24(1), e27487. doi:10.2196/27487
- Sarhaddi F et al A. comprehensive accuracy assessment of Samsung smartwatch heart rate and heart rate variability. PLoS ONE. 2022;17(12), e0268361. doi:10.1371/journal.pone.0268361
- Rowan SP, Lilly CL, Claydon EA, et al. Monitoring. one heart to help two: heart rate variability and resting heart rate using wearable technology in active women across the perinatal period. BMC Pregnancy and Childbirth. 2022;22(1), 887. doi:10.1186/s12884-022-05183-z
- Cao R, Azimi I, Sarhaddi F, et al. Accuracy Assessment of Oura Ring Nocturnal Heart Rate and Heart Rate Variability in Comparison With Electrocardiography in Time and Frequency Domains: Comprehensive Analysis. Journal of Medical Internet Research. 2022;24(1):e27487. doi:10.2196/27487; Sarhaddi F, Kazemi S, Azimi I, et al. A comprehensive accuracy assessment of Samsung smartwatch heart rate and heart rate variability. PLoS ONE. 2022;17(12):e0268361. doi:10.1371/journal.pone.0268361
- Maciel BC, Gallo Junior L, Marin Neto JA, et al. Parasympathetic contribution to bradycardia induced by endurance training in man. Cardiovascular Research. 1985;19(10):642-648. doi:10.1093/cvr/19.10.642; D’Souza A, Bucchi A, Johnsen AB, et al. Exercise training reduces resting heart rate via downregulation of the funny channel HCN4. Nature Communications. 2014;5:3775. doi:10.1038/ncomms4775; Yamamoto K, Miyachi M, Saitoh T, et al. Effects of endurance training on resting and post-exercise cardiac autonomic control. Medicine and Science in Sports and Exercise. 2001;33(9):1496-1502. doi:10.1097/00005768-200109000-00012
- Lin JL, Chan HL, Du CC, et al. Long-term. beta-blocker therapy improves autonomic nervous regulation in advanced congestive heart failure: a longitudinal heart rate variability study. American Heart Journal. 1999;137(4 Pt 1), 658-665. doi:10.1016/s0002-8703(99)70219-x
- Tankeu AT, Azabji-Kenfack M, Nganou CN, et al. Effect of propranolol on heart rate variability in hyperthyroidism. BMC Research Notes. 2018;11(1):151. doi:10.1186/s13104-018-3224-x
- Baumert M, Schmid P, Hauser AM, et al. Heart rate variability, blood pressure variability, and baroreflex sensitivity in overtrained athletes. Clinical Journal of Sport Medicine. 2006;16(5):412-417. doi:10.1097/01.jsm.0000244610.34594.07
- Baumert M et al Heart. rate variability. 2006;blood pressure variability, and baroreflex sensitivity in overtrained athletes. Clinical Journal of Sport Medicine, 16(5), 412-417. doi:10.1097/01.jsm.0000244610.34594.07
- Mourot L et al Decrease. in heart rate variability with overtraining: assessment by the Poincaré plot analysis. Clinical Physiology and Functional Imaging. 2004;24(1), 10-18. doi:10.1046/j.1475-0961.2003.00523.x
- Koerber D, Khan S, Shamsheri T, et al. Accuracy of Heart Rate Measurement with Wrist-Worn Wearable Devices in Various Skin Tones: a Systematic Review. Journal of Racial and Ethnic Health Disparities. 2023;10(6):2676-2684. doi:10.1007/s40615-022-01446-9
- Amekran Y, El Hangouche AJ. Effects of Exercise Training on Heart Rate Variability in Healthy Adults: A Systematic Review and Meta-analysis of Randomized Controlled Trials. Cureus. 2024;16(6):e62465. doi:10.7759/cureus.62465
- Jensen MT, Wod M, Galatius S, et al. Heritability of resting heart rate and association with mortality in middle-aged and elderly twins. Heart. 2018;104(1):30-36. doi:10.1136/heartjnl-2016-310986
- van de Vegte YJ, Eppinga RN, van der Ende MY, et al. Genetic. insights into resting heart rate and its role in cardiovascular disease. Nature Communications. 2023;14(1), 4646. doi:10.1038/s41467-023-39521-2
- Carlson N, Dixen U, Marott JL, et al. Predictive. value of casual ECG-based resting heart rate compared with resting heart rate obtained from Holter recording. Scandinavian Journal of Clinical and Laboratory Investigation. 2014;74(2), 163-169. doi:10.3109/00365513.2013.867531
- Kinnunen H, Rantanen A, Kenttä T, et al. Feasible. assessment of recovery and cardiovascular health: accuracy of nocturnal HR and HRV assessed via ring PPG in comparison to medical grade ECG. Physiological Measurement. 2020;41(4), 04NT01. doi:10.1088/1361-6579/ab840a
- Rehman RZU, Del Din S, Shi JQ, et al. Assessment of Physiological Signals from Photoplethysmography Sensors Compared to an Electrocardiogram Sensor: A Validation Study in Daily Life. Sensors (Basel). 2024;24(21). doi:10.3390/s24217022
- O’Neal WT, Chen LY, Nazarian S, et al. Reference. ranges for short-term heart rate variability measures in individuals free of cardiovascular disease: The Multi-Ethnic Study of Atherosclerosis (MESA). Journal of Electrocardiology. 2016;49(5), 686-690. doi:10.1016/j.jelectrocard.2016.06.008
- Ortega E, Bryan CYX, Christine NSC. The Pulse of Singapore: Short-Term HRV Norms. Applied Psychophysiology and Biofeedback. 2024;49(1):55-61. doi:10.1007/s10484-023-09603-4
- El-Malahi O et al Beneficial. impacts of physical activity on heart rate variability: A systematic review and meta-analysis. PLoS ONE. 2024;19(4), e0299793. doi:10.1371/journal.pone.0299793
- Picard M, Ginoux C, Grassen Barbeau G, et al. Effect of exercise training on heart rate variability in type 2 diabetes mellitus patients: A systematic review and meta-analysis. PLoS ONE. 2021;16(5):e0251863. doi:10.1371/journal.pone.0251863
- Tsuji H, Venditti FJ Jr, Manders ES, et al. Reduced. heart rate variability and mortality risk in an elderly cohort. The Framingham Heart Study. Circulation. 1994;90(2), 878-883. doi:10.1161/01.cir.90.2.878
- Vinik AI, Maser RE, Mitchell BD, et al. Diabetic. autonomic neuropathy. Diabetes Care. 2003;26(5), 1553-1579. doi:10.2337/diacare.26.5.1553


